

Osteochondritis dissecans (OCD), a progression of osteochondrosis, is a joint condition in young, growing dogs where cartilage fails to form properly, causing pain and lameness. It can occur in a variety of joints, most often the shoulder, elbow, stifle, or hock.
Osteochondrosis is a disorder in which the normal process of cartilage turning into bone (endochondral ossification) is disrupted in a growing dog. When a section of this abnormal cartilage cracks or separates from the underlying bone, it forms a loose or partially attached flap — a stage called osteochondritis dissecans (OCD). This flap causes joint irritation, inflammation, and mechanical interference with movement, resulting in pain and lameness.
OCD is more common in large and giant breeds, and genetic predisposition plays a major role. Other contributing factors include rapid growth, diets high in calcium or calories, repetitive joint stress, and hormonal influences.
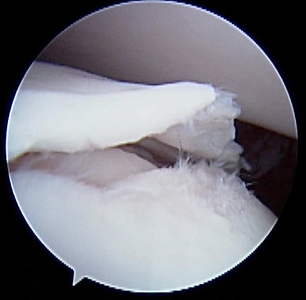
Arthroscopic image of an OCD flap.
Osteochondrosis itself does not usually cause symptoms because the cartilage remains intact and does not irritate the joint. If it progresses to OCD, the cartilage flap creates irritation and inflammation, nearly always leading to persistent pain and limping.
Clinical signs most often appear in young, growing dogs (6–18 months). In some cases, OCD can also contribute to lameness in older dogs as secondary arthritis develops.
OCD lesions are usually visible on good-quality radiographs (X-rays), especially in typical joint locations. CT scans may be used to better define the size, shape, and exact location of the defect — helpful for surgical planning. Arthroscopy allows direct visualization of the lesion and confirmation of cartilage flap formation.
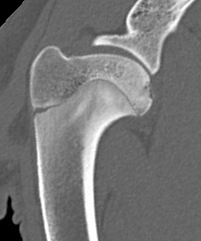
CT scan of a dog shoulder showing an OCD lesion (star).
Osteochondrosis without pain or inflammation generally does not require surgery and can be monitored over time. However, OCD almost always causes persistent lameness, and removing the cartilage flap typically leads to improvement — though outcomes vary by joint.
Surgery can be performed either through an open approach or using minimally invasive arthroscopy, which often results in faster recovery and less postoperative discomfort. In cases where the defect is large, resurfacing techniques such as grafting or synthetic implants may be used to restore a functional joint surface.
Prognosis depends on the joint involved, the size of the lesion, and how long the condition has been present. Shoulder OCD generally has the best outcome, while hock (ankle) lesions respond less predictably.
Larger defects leave less healthy cartilage to protect the joint, which can worsen the long-term outlook. Nearly all cases eventually develop some degree of secondary osteoarthritis, which may or may not cause ongoing issues but can lead to long-term joint stiffness in some dogs.
Medial shoulder instability (MSI) is being diagnosed more frequently, particularly in highly active dogs. Repetitive strain and accelerated wear on the joint’s stabilizing structures can lead to lameness and reduced performance.
Medial shoulder instability (MSI) occurs when the structures that stabilize the inner (medial) side of a dog’s shoulder become stretched or torn, most often from repetitive strain. The shoulder is a ball-and-socket joint, with the ball (humeral head) fitting into the socket (glenoid) and held in place by ligaments, a joint capsule, and surrounding muscles.
The medial glenohumeral ligament is the main supporting structure of the joint, and damage to this ligament or nearby tissues allows the humeral head to shift excessively. MSI is most common in highly active dogs such as agility and working dogs and is therefore seen more often in medium to large sporting breeds, although any athletic dog may be affected. Concurrent arthritis is frequently present.
Symptoms often develop gradually but may also appear suddenly without a specific injury. Affected dogs typically limp, with lameness that worsens after exercise or, in some cases, after rest. Reduced performance—such as reluctance to jump or difficulty turning sharply—is also common.
Testing for MSI begins with a careful orthopedic exam, but diagnosing shoulder problems can be challenging. The shoulder may not be obviously painful, so other common causes of lameness must first be ruled out.
A sedated orthopedic exam can provide additional information, though joint angle measurements are not highly reliable. Ultrasound can detect some structural problems, such as biceps or supraspinatus tendinopathy. MRI gives excellent soft-tissue detail but is costly and not always necessary.
Arthroscopy remains the gold standard for diagnosing MSI because it allows direct visualization of the medial shoulder structures. Needle arthroscopy is an even less invasive technique that can often be performed under sedation, providing outstanding detail while minimizing cost and recovery time.
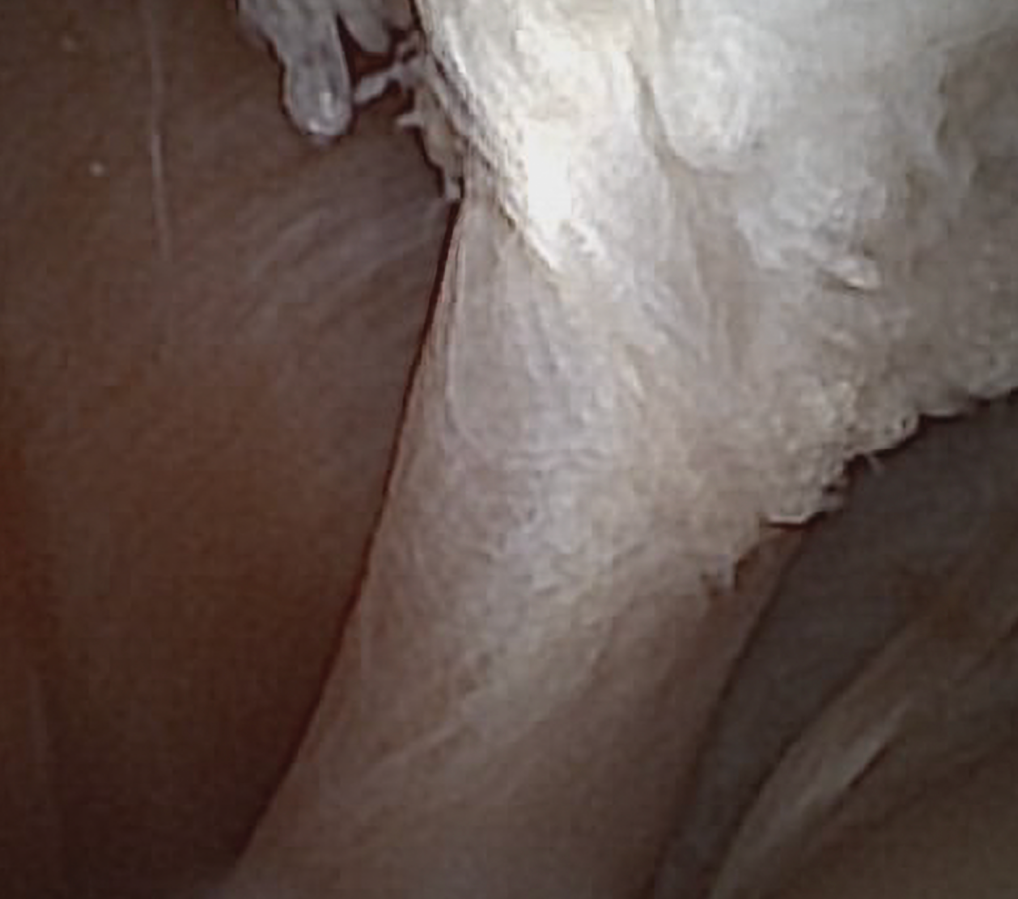
Needle scope image of the biceps tendon inside the joint
Treatment usually begins with conservative management aimed at reducing strain on the shoulder and allowing irritated tissues to recover. This may include:
If lameness persists or instability is moderate to severe, surgical stabilization may be recommended. Surgical options focus on tightening or reconstructing the damaged ligaments and joint capsule to restore normal stability. Post-operative rehabilitation is essential for the best outcome.
Prognosis for MSI varies widely depending on the severity of ligament damage, the presence of arthritis, success of rehabilitation, and whether surgical stabilization is required. Dogs with mild instability often improve with conservative treatment, while moderate or severe MSI may require surgery for long-term improvement.
Most dogs can return to comfortable daily activity, and many athletic dogs regain good performance. However, chronic or advanced cases, especially those with secondary arthritis, may have a more guarded long-term outlook.
At Animal Orthopaedic Clinic of Florida, diagnosing shoulder conditions like MSI requires a combination of specialized orthopedic examination and advanced diagnostic tools. Techniques such as needle arthroscopy allow us to directly evaluate the joint with minimal invasiveness.
Because treatment success depends on understanding the exact structures involved, your pet’s lifestyle, and your goals, we work closely with you to create a personalized plan that gives your dog the best chance at full, comfortable function.
Medial shoulder luxation is a condition that develops without a major injury, most often in small-breed dogs, where the shoulder dislocates inward. It typically causes severe and persistent lameness or complete avoidance of limb use.
Medial shoulder luxation occurs when the head of the upper forelimb bone (humerus) slips out of the shoulder socket (glenoid) toward the inside, often with little or no apparent trauma. It is believed to be related to how the joint developed, leading to looseness and gradual degeneration over time. Eventually, this instability can cause a sudden full dislocation.
In some cases, the shoulder may not fully dislocate but becomes so unstable that it cannot function normally. The condition is most common in older, small, and toy breed dogs.
Dogs with medial shoulder luxation typically hold the affected leg up close to their body and refuse to bear weight, or may only toe-touch with the limb. Because the shoulder is deeply surrounded by muscle, it often appears normal externally even though the joint is unstable or dislocated.
In partial luxations, dogs may still place the paw on the ground but will limp noticeably or have intermittent lameness that worsens with activity.
Diagnosis begins with a thorough physical and orthopedic examination. An experienced veterinarian can often suspect the problem based on the way the joint moves and feels. Under sedation or anesthesia, the shoulder may move easily in and out of position, confirming instability.
Radiographs (X-rays) typically reveal the dislocation and may show abnormal joint shape contributing to the issue. In some cases, stress radiographs are taken to demonstrate joint looseness more clearly.
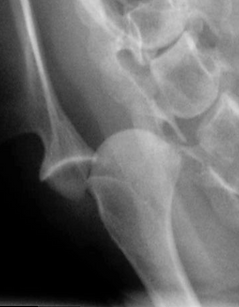
Radiograph showing medial shoulder luxation.
Treatment for medial shoulder luxation almost always involves surgery. The goal is to either stabilize the joint or fuse it permanently (arthrodesis), depending on the severity and chronicity of the condition.
The choice of procedure depends on multiple factors, including joint shape, duration of instability, size of the dog, and the presence of degenerative changes.
Prognosis is generally good, though it varies based on the procedure and individual patient factors. Stabilization procedures preserve motion but carry the risk of re-luxation. Arthrodesis removes that risk but can be associated with complications such as implant failure or delayed healing.
When the joint remains stable after reconstruction or heals fully following fusion, most owners report excellent comfort and functional mobility in their pets.
Osteoarthritis is an extremely common problem in both dogs and cats. In some animals, it is very well tolerated and causes minimal issues, while in others, it can be debilitating. Prevention and treatment recommendations are highly individualized.
Osteoarthritis is also known as degenerative joint disease (DJD), arthritis, or osteoarthrosis. The main feature is the thinning and wearing of cartilage, but it also affects other joint tissues, including bone, ligaments, the joint capsule, and surrounding muscles. As the joint degenerates, the underlying bone can become exposed and both soft and hard tissues may thicken. The result is a joint that no longer glides smoothly or moves through its full range of motion.
In dogs, osteoarthritis is usually secondary — developing as a consequence of another joint issue such as a ligament injury, fracture, or developmental disorder like elbow or hip dysplasia. Because secondary OA is so prevalent, identifying and addressing the underlying cause is essential for effective treatment planning.
Classic symptoms of osteoarthritis include:
In cats, signs are often more subtle — such as reduced movement around the home, avoiding touch, or less grooming. Importantly, many animals with osteoarthritis show no outward symptoms at all.
A careful orthopedic examination is crucial. Affected joints may show thickening, reduced range of motion, pain, or crepitus (a crunchy sensation). Multiple joints may be involved, so a thorough evaluation is essential.
Determining the underlying cause is just as important — for example, instability in an arthritic stifle can suggest secondary arthritis due to a cranial cruciate ligament rupture.
Radiographs (X-rays) are vital for confirming osteoarthritis, identifying the cause, and gauging severity. In some cases, CT or MRI can provide more detail about bone and soft-tissue changes. Arthroscopy allows direct visualization inside the joint and can sometimes be used for treatment as well as diagnosis.
The goal of treatment is to reduce pain, improve movement, and slow further damage. Osteoarthritis is frequently managed medically through anti-inflammatory medication, weight control, joint supplements, and physical therapy. Many pets can remain comfortable for years with these measures alone.
Surgical options may be recommended for specific reasons:
The most appropriate approach depends on the affected joint, disease severity, and the pet’s overall health and activity level.
Most dogs can enjoy many years of excellent quality of life with the right management plan. The progression of osteoarthritis varies — some dogs show minimal issues, while others develop more significant mobility limitations over time.
Early diagnosis and proactive care — including weight control, tailored exercise, pain management, and appropriate surgical intervention — can dramatically slow progression and improve comfort and mobility.