

Elbow dysplasia is the leading cause of forelimb lameness in medium to large dogs.
It’s an umbrella term for several developmental problems in the elbow that all lead to joint
incongruity, cartilage damage, pain, and progressive arthritis.
Elbow dysplasia is a developmental disorder that arises while a young dog’s bones and
joints are still forming. In affected dogs, the components of the elbow joint do not grow together in
perfect alignment, creating abnormal forces and uneven wear within the joint. Over time, this results
in cartilage injury, pain, and reduced mobility.
The condition is thought to involve a combination of genetic and environmental factors
and most often affects medium to large breeds such as Labradors, Golden Retrievers, German Shepherds,
and Rottweilers. Both elbows are frequently involved, although not always to the same degree.
The elbow joint is complex, and several key structures can be affected:
<!– Optional image row – add images if/when available
Elbow dysplasia may cause a gradual onset of lameness as changes progress over time,
or a more sudden onset without any obvious injury. Common signs include stiffness,
reduced willingness to play, and exercise intolerance. Lameness may be worse after
activity, after rest, or present constantly.
The severity of symptoms can vary widely and does not always reflect the extent of
joint damage. Some dogs remain active with only mild limitations, while others are significantly
impaired. As osteoarthritis progresses, signs typically become more obvious over time.
A thorough orthopedic examination is essential to localize the problem, assess pain,
range of motion, and overall limb function, and detect any additional issues. Because elbow dysplasia
can occur alongside other developmental joint disorders (such as hip dysplasia), we also evaluate for
abnormalities in other limbs.
Radiographs (X-rays) are usually performed first and often show characteristic
changes, although some lesions—especially FCP—can be difficult to see. In many cases, a
CT scan is recommended to better characterize the problem and identify subtle
changes in bone.
Arthroscopy (keyhole surgery to look directly inside the joint) is particularly
valuable, since cartilage cannot be seen on X-rays or CT. Arthroscopy allows direct evaluation of the
cartilage surfaces and loose fragments and can be combined with treatment in the same procedure.
<!– Optional arthroscopy image
Treatment for elbow dysplasia depends on the specific lesion, the degree of
arthritis, and how severely the dog is affected.
In dogs with more advanced arthritis, “unloading” procedures such as proximal
abducting ulnar osteotomy (PAUL) or sliding humeral osteotomy (SHO) may be considered to shift weight
away from the most damaged areas of the joint. Total elbow replacement is also an option in selected
dogs, but it is highly technical and long-term outcomes are still being defined. Overall, surgery can
help in carefully chosen cases, but there is no perfect fix for elbow dysplasia.
Because of these limitations, medical management is often the preferred approach for
many dogs. This typically includes a combination of weight control, controlled exercise, joint
supplements, anti-inflammatory and pain medications, and physical rehabilitation.
Prognosis varies widely and depends on the type of lesion, the severity of joint
changes, and how advanced the arthritis is at diagnosis. Some dogs remain active for
years with minimal limitations, while others develop progressive lameness despite treatment.
Even with surgery, arthritis usually progresses over time, and a complete cure is not expected.
However, long-term pain control and functional comfort are realistic goals for many
dogs, especially when a thoughtful treatment plan is followed and weight and activity are managed
carefully.
At Animal Orthopaedic Clinic of Florida, we base our recommendations on the
best available evidence, the specific features of your dog’s elbows, and your goals
and expectations. We understand the limitations of surgery for elbow dysplasia and offer it only when
we believe it has a better chance of helping than medical management—which is relatively uncommon.
Our advice is guided by honesty, not procedure volume. With extensive experience in
diagnosing and managing elbow dysplasia, including research and teaching on this condition, you can
rely on us to help you choose the most appropriate, realistic plan for your dog.
Humeral condylar fractures are one of the most common fore limb injuries in dogs. Prompt surgical repair is essential for the best long-term outcomes.
Humeral condylar fractures are breaks at the lower end of the humerus (upper fore limb bone) where it forms part of the elbow joint. This area has two rounded surfaces, or condyles — the medial and lateral — and the fracture can involve just one side (unicondylar) or split through both (bicondylar).
These injuries are relatively common in certain breeds and can occur even from low-impact events like falling or jumping down from furniture. Young dogs and breeds such as French Bulldogs are overrepresented. Spaniel breeds may also be affected due to
Humeral Intracondylar Fissure (HIF), where an incomplete fusion weakens the bone and predisposes it to fracture.
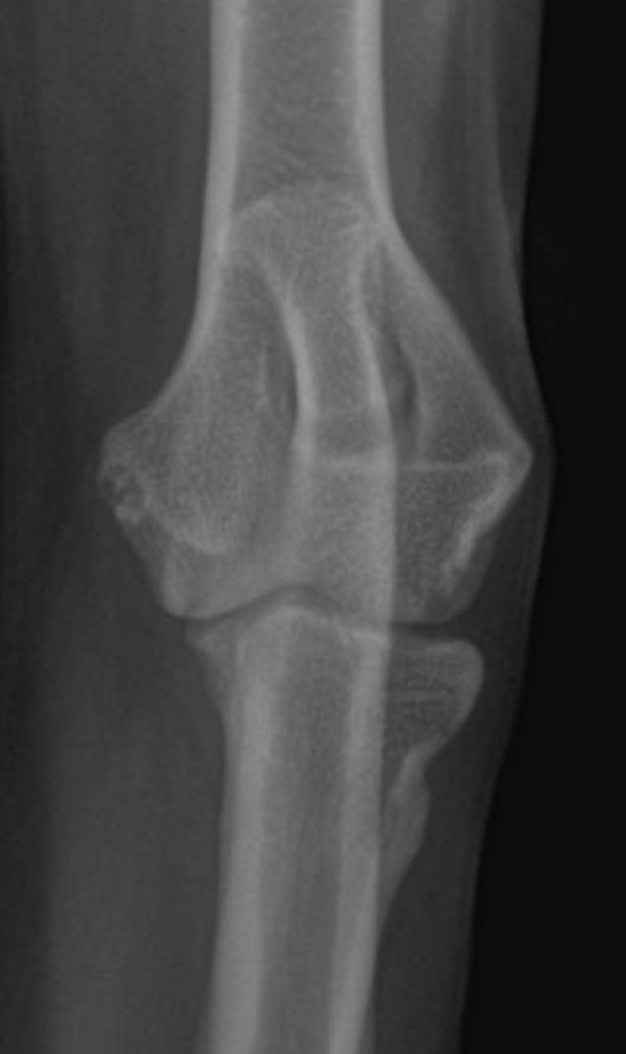
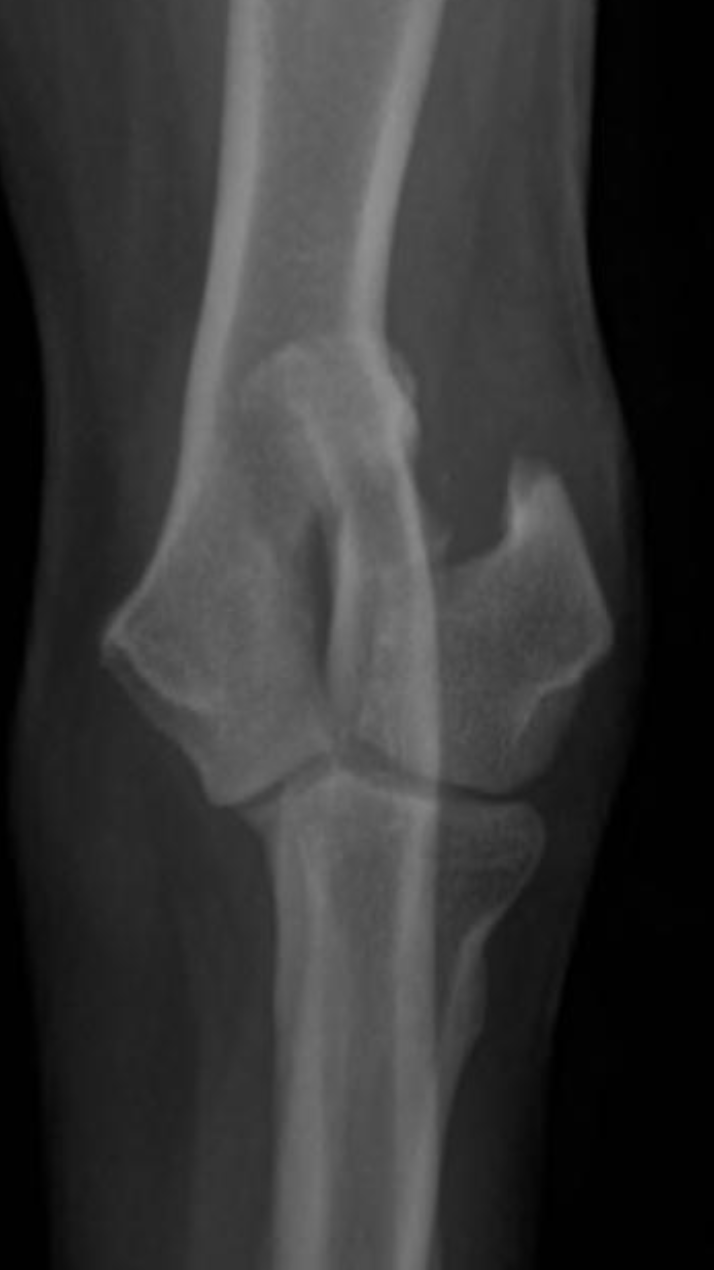
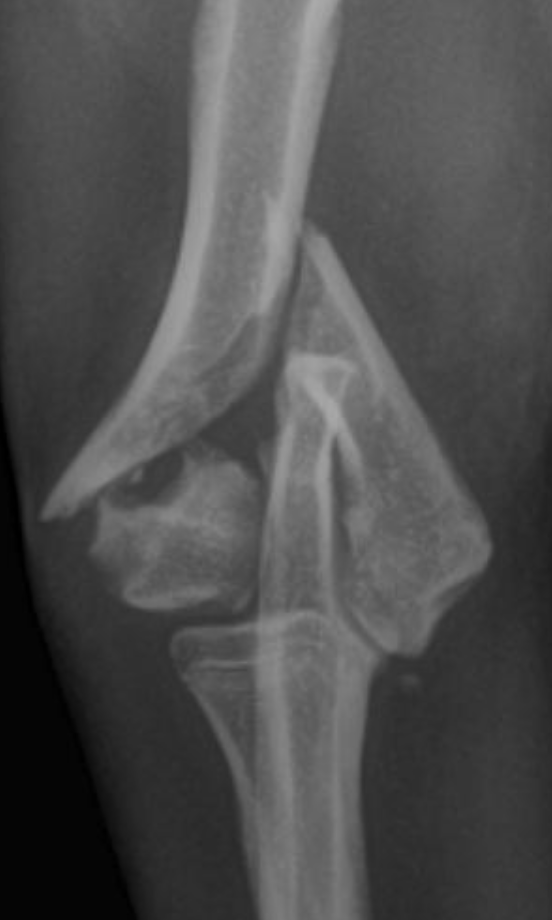
Dogs with humeral condylar fractures typically show sudden, severe limping after a fall or jump. The elbow is often very sensitive to touch, and the dog may hold the leg up and refuse to use it.
Diagnosis begins with an orthopedic exam. High-quality radiographs are essential. If the fracture is complex — particularly bicondylar fractures or suspected Humeral Intracondylar Fissure (HIF) — a CT scan may be recommended for a more complete view.
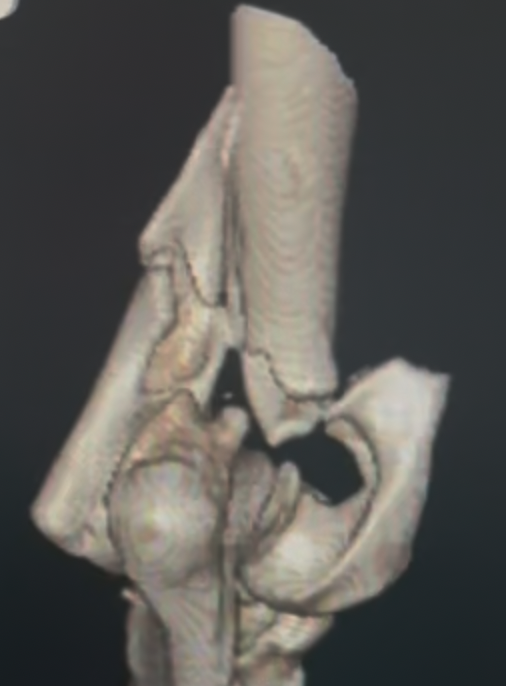
Prompt and accurate repair is critical. Surgery typically involves placement of a transcondylar screw to stabilize the fracture, often paired with plates or pins for additional support. Bicondylar fractures are especially challenging because the elbow is effectively split into three pieces, requiring meticulous reconstruction.
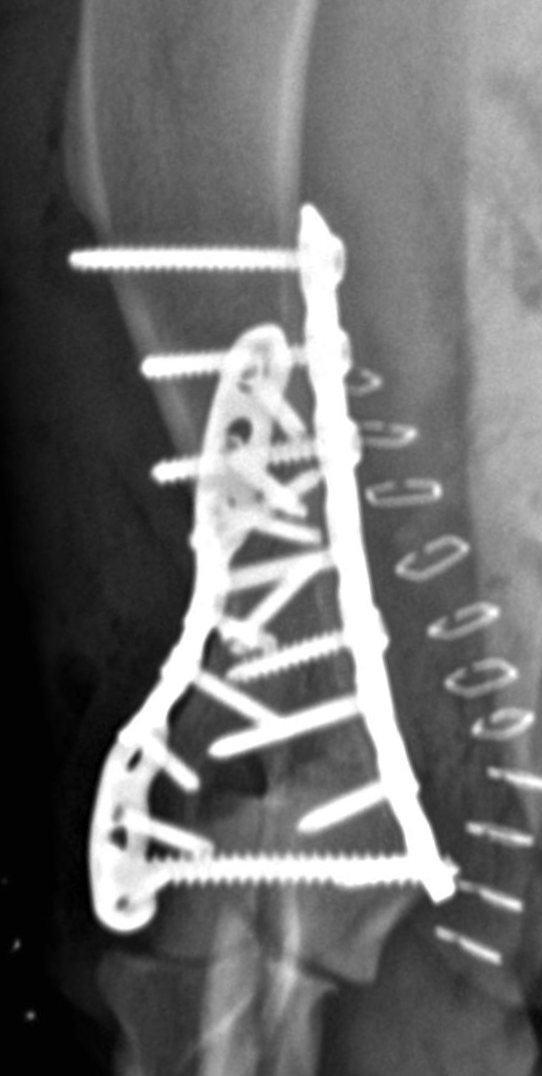
Humeral condylar fractures require surgeons with extensive experience and specialized tools. At AOCF, advanced imaging (CT and fluoroscopy) helps us understand the fracture before and during surgery. We maintain a full range of implants for even the most complex repairs and use minimally invasive techniques when appropriate. This approach ensures precise reconstruction, faster recovery, and the best possible long-term outcome for your pet.
Twisting, bending, and deviating limbs are not uncommon in dogs and cats.
Limb deformities occur when a bone grows or heals abnormally, causing it to angle, twist, turn, deviate, or shorten. These changes usually arise from growth plate problems due to
genetics (as in Dachshunds and other chondrodystrophic breeds), trauma that damages a growth plate, or bones that heal improperly after a fracture (malunions).
Depending on severity, deformities may cause visible limb dysfunction and, if the joints are affected, can lead to arthritis. In some dogs, however, mild deformities cause little to no noticeable problem.

Limb deformities are usually obvious when there is visible bending or twisting of a leg, which may gradually worsen over time. Different bones can be affected, and deformities may lead to limping — either from abnormal mechanics or from soreness in the affected limb.
Evaluation begins with a comprehensive orthopedic examination. Your pet’s gait is observed to assess limb function and balance. The affected limb is then carefully examined to check alignment, measure length, and detect any pain or joint changes.
Radiographs (X-rays) are the most important initial diagnostic tool. They are taken from multiple angles and often include the opposite limb for comparison. In more complex cases, a CT scan may be performed to create a 3D model of the bones, allowing precise surgical planning. If surgery is anticipated, routine bloodwork and urinalysis are also done to ensure your pet is healthy for anesthesia.
Not all limb deformities require surgery. Mild deformities that cause little or no discomfort can often be monitored over time, especially if your pet is functioning well.
In young, growing dogs, carefully timed procedures such as partial bone excision (ostectomy) may allow the limb to correct itself naturally as growth continues. For more significant deformities — especially those causing pain, limping, or risk of joint degeneration — a corrective osteotomy is usually recommended. In this procedure, the bone is precisely cut, realigned to restore normal mechanics, and stabilized using plates, screws, or external fixators.
In advanced or highly complex cases, 3D-printed surgical guides and detailed pre-operative computer modeling may be used to plan the correction with extreme accuracy.
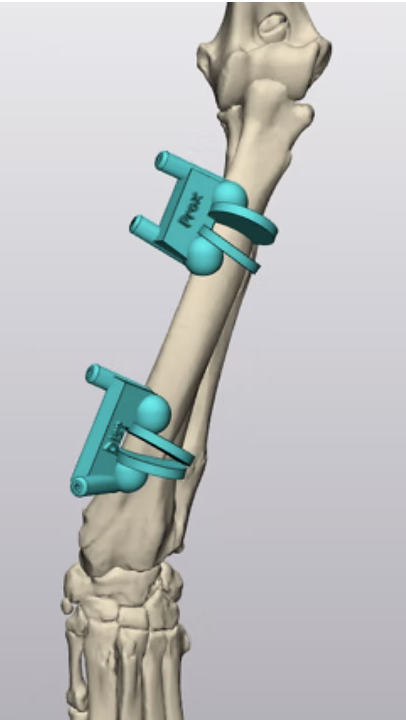
The outlook for recovery from a limb deformity varies widely depending on severity, age, and overall health. Mild cases can have excellent long-term outcomes without intervention, while severe deformities may require complex surgical correction.
Successful outcomes rely on accurate surgical technique, proper implants, and careful post-operative management. With expert planning and follow-up, most dogs and cats regain comfortable function and improved limb alignment after corrective surgery.
Osteoarthritis is an extremely common problem in both dogs and cats. In some animals, it is well tolerated and causes minimal issues, while in others it can be debilitating. Prevention and treatment recommendations are highly individualized.
Osteoarthritis — also known as degenerative joint disease, arthritis, or osteoarthrosis — is characterized by thinning and wearing of cartilage. It also affects other joint tissues including bone, ligaments, the joint capsule, and surrounding muscles. As the joint degenerates, the underlying bone can become exposed and both soft and hard tissues may thicken. The result is a joint that cannot glide smoothly through a full range of motion.
In dogs, osteoarthritis is usually secondary — meaning it develops as a consequence of another joint problem such as ligament injury, fracture, or developmental disorders like elbow or hip dysplasia. Because secondary OA is so common, identifying and addressing the underlying problem is critical for developing the best treatment strategy.
Classic symptoms of osteoarthritis include:
In cats, signs are often more subtle — such as reduced movement around the home, avoiding touch, or grooming less frequently. Importantly, many animals with osteoarthritis show no obvious symptoms at all.
A careful orthopedic examination is crucial. Affected joints may show thickening, reduced range of motion, pain, or crepitus (a crunching sensation). Multiple joints may be involved, so a thorough exam is essential.
It’s also important to determine any underlying cause. For example, instability in an arthritic stifle may indicate secondary arthritis from a cranial cruciate ligament rupture.
Radiographs (X-rays) are very important for confirming osteoarthritis, identifying the cause, and gauging severity. In some cases, advanced imaging such as CT or MRI can reveal more detail about bone and soft tissue changes. Arthroscopy allows direct visualization of the joint interior and can be used both for diagnosis and treatment of certain causes of secondary OA.
The primary goals are to reduce pain, improve movement, and slow further damage. Osteoarthritis is often managed medically through anti-inflammatory medications, weight control, joint supplements, and physical therapy. Many pets remain comfortable for years with these measures alone.
Surgical options may be recommended for a variety of reasons:
The best approach depends on the joint involved, the severity of disease, your pet’s overall health, and activity level.
Most dogs can enjoy many years of good quality life with the right management plan. The course of the disease varies — some dogs remain asymptomatic for life, while others develop more significant mobility issues over time.
Early diagnosis and proactive care — including weight control, tailored exercise, pain management, and, when appropriate, surgical intervention — can slow progression and greatly improve comfort and mobility.
At Animal Orthopaedic Clinic of Florida, every patient benefits from unmatched expertise. Our head surgeon is an internationally recognized leader and researcher in elbow disorders. Using evidence-based, individualized care, we are dedicated to giving your dog the best chance at long-term, pain-free mobility.
Kim SE*, Pozzi A, Yeh JC, Lopez M, Au Yong J, Townsend S, Dunlap AE, Christopher SA, Lewis DD, Johnson MD, Petrucci K. Evaluation of intra-articular umbilical cord derived mesenchymal stem cells for the treatment of chronic elbow osteoarthritis in dogs. Frontiers in Veterinary Science 2019; 6:474.
Coggeshall JD, Reese DJ, Kim SE, Pozzi A. Arthroscopic-guided ulnar distraction for the correction of elbow incongruency in four dogs (five elbows). J Small Anim Pract 2014; 55:46–51.
Cuddy LC, Lewis DD, Kim SE, Conrad BP, Banks SA, Horodyski M, Fitzpatrick N, Pozzi A. Ex vivo contact mechanics and three-dimensional alignment of normal dog elbows after proximal ulnar rotational osteotomy. Vet Surg 2012; 41(8):905–914.
Cuddy LC, Pozzi A, Lewis DD, Conrad BP, Horodyski MB, Kim SE, Fitzpatrick N. Contact Mechanics and Three-Dimensional Alignment of Normal Dog Elbows. Vet Surg 2012; 41(7):818–828.